Sometimes people experience bouts of inflammation known as ‘flares’, which can be associated with swelling of the knee. OA of the knee typically presents with pain and stiffness after long periods without moving such as first thing in the morning or after sitting for long periods which can be associated with audible noises such as clicking or creaking. Activities such as standing for long periods going up and down stairs and bending the knee beyond 90° (right angles) making squatting or kneeling challenging. This can start to impact on an individual’s quality of life making even tasks we normally take for granted a real challenge.
Strength-based exercise for the major muscle groups of the lower limb has been shown to be a very effective treatment and is indeed considered the gold standard first line treatment. The key is to do the correct exercises consistently enough to have a positive effect. Losing weight also seems to assist in easing peoples symptoms and well-fitting and cushioned footwear can give further relief. Despite taking these measures, many people experience difficulty with their knees. Joint replacement surgery can be a good option for people, however orthopaedic surgeons will often be reluctant to consider knee replacement in the early stages. Some emerging evidence suggests that keyhole surgery, which was previously utilised for knee OA, may not be particularly helpful and indeed could contribute to the acceleration of the OA process. This could leave people thinking that they are out of options and that they just have to manage their pain. There are however some additional options in the form of therapeutic joint injections.
Steroid (corticosteroid or ‘cortisone’) injections, which provide a strong anti-inflammatory effect, can provide some temporary relief of symptoms if the knee is undergoing an inflammatory ‘flare’ as mentioned above. However, steroid injections are also known to have a long term negative impact on the knee cartilage if given in too high a dosage or too frequently so they should be used with caution. Another option is a
hyaluronic acid injection. Hyaluronic acid is the largest component of the joint lubricant (synovial fluid) and is a viscous substance that provides lubrication and shock absorption and can provide good relief for people who have mild to moderate knee OA. There is some evidence to support the effectiveness of hyaluronic acid injections and importantly they don’t seem to have any negative impact on the health of the knee in the long term. So how do you know which option is for you?
At Life Fit, we offer a
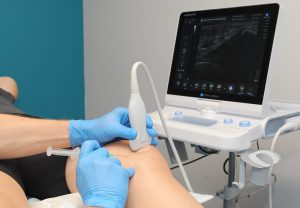
one-stop clinic where you will be offered a full clinical and functional assessment, an ultrasound scan, and the options of physiotherapy-based rehabilitation, steroid and hyaluronic acid injections. There is no substitute for a thorough and expert clinical examination, however the addition of the ultrasound examination can give further valuable information regarding the swelling and inflammatory status of the knee thus enhancing the diagnosis and treatment choice. You can read more here.