Greater Trochanteric Pain Syndrome / Trochanteric Bursitis
There are several names given to pain experienced on the outside of the hip. Namely, trochanteric bursitis, gluteal tendinopathy (tendinitis), and greater trochanteric pain syndrome (GTPS). GTPS is the more contemporary term and reflects the multi factorial nature of this presentation. Typically patients will experience pain with an epicentre at the bony prominence on the outside of the hip, known as the greater trochanter. In some circumstances it can also cause referred pain down the outside of the thigh. It is often a relief for patients to learn that this is not the hip joint and is the attachment point for two of the tendons belonging to gluteal muscles. The term trochanteric bursitis is now seen to be out-dated as modern research has illustrated that this is primarily a tendon issue, however a bursa (a small membrane sac next to the tendons) can become irritated and swollen as a result. Although the most commonly affected bursa is called the ‘trochanteric bursa’ there are in fact many bursae around this region of the hip.
Although this is not an issue with the hip joint, symptoms can be quite limiting and pain can persist for some time. It is more common in females and can have a relationship with the menopause. Other factors that can contribute to the problem are a change in normal activities (i.e. taking up a new activity such as hillwalking or running), sitting in cross-legged positions and inappropriate stretching of the gluteal muscles. Once the issue is established, patients can often find that sleeping positions aggravate their symptoms causing sleep disturbance. Initial walking or movement following a period of inactivity, especially if the hip has been in a flexed position, can cause ‘start-up’ pain. While these symptoms tend to ease off with some movement, prolonged walking or running, especially up hills, can result in further aggravation with pain returning either into the activity or on stopping; sometimes later on that day or into the next day.
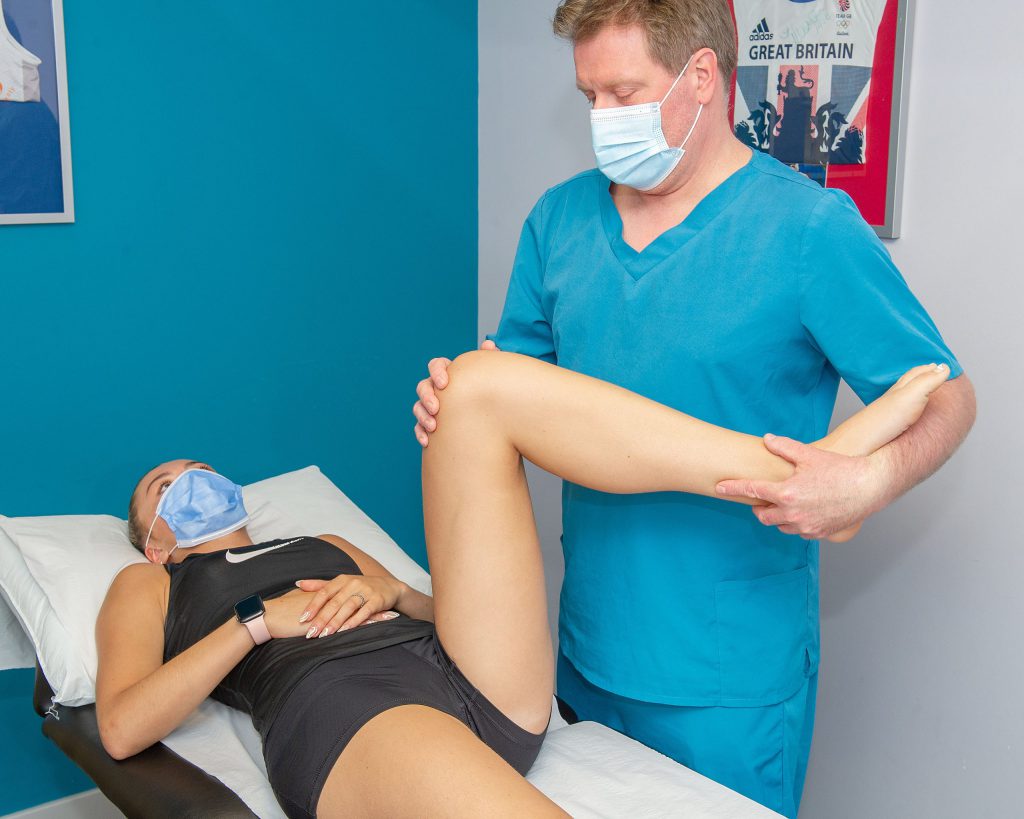
The first line treatment choice is physiotherapy-based management. A physiotherapist experienced in treating these issues will be able to fully assess the problem and differentiate between GTPS and other conditions affecting this area. Occasionally an ultrasound scan can be used to assess the tendons and bursa to determine the most appropriate treatment. Physiotherapy will be centred around designing and undertaking the most appropriate exercises. Historically stretching of the gluteal muscles was thought to be of benefit, however we now understand that this can further aggravate the issue, possibly delaying recovery. Any contributory factors, such as issues with the low back or biomechanics, will also be addressed alongside specific gluteal exercises to promote recovery. In addition to what patients should be doing, the physiotherapist will discuss which positions and activities to avoid, reduce or modify in order to maximise the effectiveness of the rehabilitation program. Manual therapy, such as massage, may also be applied to assist with pain relief and to assist in improving limitations in movement.
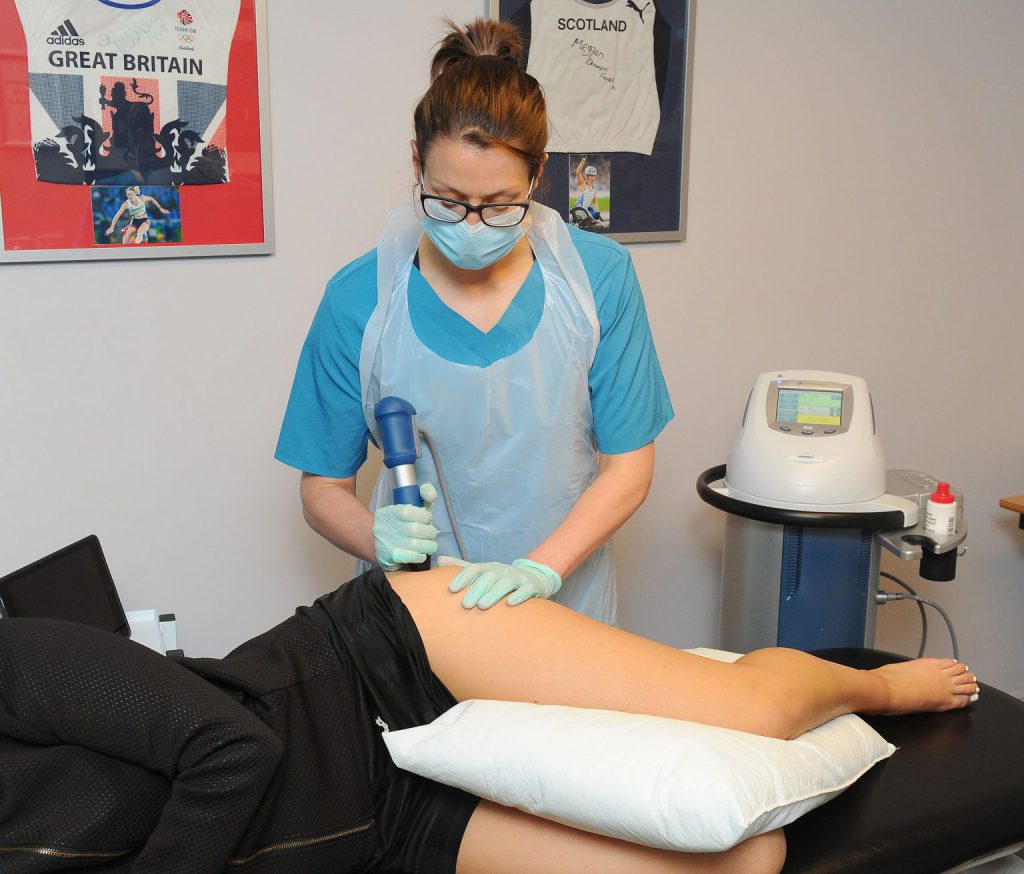
Greater trochanteric pain syndrome can be a stubborn problem. In resistant cases, shockwave therapy can be considered alongside a physiotherapy program. There is good evidence to support the use of shockwave therapy in this condition. The treatment involves using a specialised machine to deliver high energy pressure waves to the affected tendon(s) which in turn encourages healing at a cellular level and is maximised by appropriate exercise. This is why having shockwave delivered by experienced physiotherapists at Life Fit Wellness is of benefit.
Previously steroid injections would be administered quite early on in the development of GTPS. We now know that steroid injections may inhibit the healing process of tendons and generally this is not seen as a first line treatment. There are some circumstances however where a steroid injection can be of benefit, in which case we advise an ultrasound-guided steroid injection targeting the bursa to specifically avoid injecting the tendon. Hyaluronic acid (Ostenil Tendon) is a lubricating agent that can be administered as an injection to facilitate recovery. It is not harmful to tendons in the way that steroid can be, however there is not the same degree of research investigating its effectiveness, that said it remains a viable treatment option for some people.